New data from one of the largest brain imaging studies of its type has found a consistent association between increased body weight and decreased cerebral blood flow. The research offers greater insights into the links between Alzheimer’s and obesity, suggesting maintaining a healthy weight can directly reduce one’s risk of developing dementia.
Prior epidemiological studies have delivered frustratingly inconsistent results when researchers have tried to determine clear links between obesity in mid-life, and the development of dementia in later-life. However, a compelling 2017 meta-study found obesity seems to be directly associated with cognitive decline, and weight loss can lead to notable improvements in cognitive function.
In a new study conducted by a team of US researchers, brain scans from more than 17,000 subjects were analyzed to investigate the association between body weight and cerebral blood flow. The patterns detected were striking, with blood flow across a number of brain regions decreasing relative to a greater body mass index.
The observed decreases in cerebral blood flow were particularly noted in five key brain regions relevant in subjects with Alzheimer’s disease – the temporal lobe, parietal lobe, hippocampus, posterior cingulate, and precuneus.
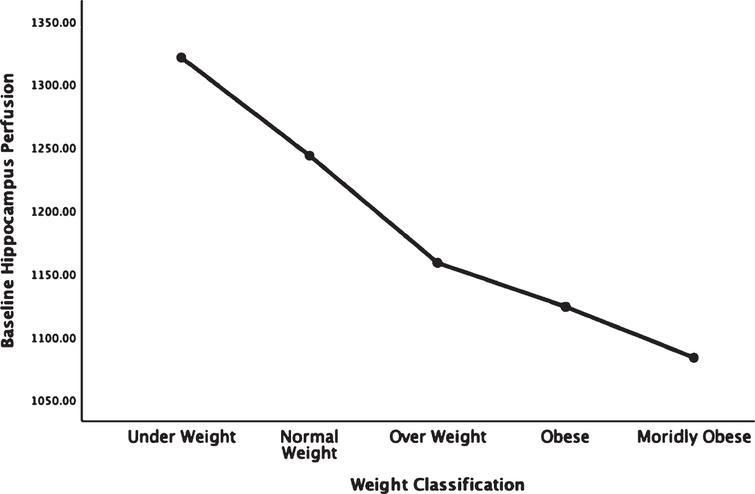
Amen et al, Journal of Alzheimer’s Disease
“This study shows that being overweight or obese seriously impacts brain activity and increases the risk for Alzheimer’s disease as well as many other psychiatric and cognitive conditions,” explains lead author on the study, Daniel Amen.
The study does not explore exactly how excess body weight could directly be causing these brain blood flow reductions but the researchers do hypothesize several potential mechanisms that could be at play. These include obesity-related changes to hormone levels or excess body weight triggering systemic inflammation.
“The relationship of obesity on brain physiology may occur through several mechanisms,” the researchers write in the study. “One is through neuroinflammation and its influence of perfusion. Obesity is a known systemic proinflammatory state. Neuroinflammation is related to cerebral hypoperfusion through pathways that include TREM-2, a biomarker for neuroinflammation also noted in AD [Alzheimer’s Disease]. Thus, chronic obesity with its associated systemic inflammation my trigger a resultant neuroinflammation and hypoperfusion.”
It is unclear what kind of long-term effects these cerebral blood flow changes confer. Again, that wasn’t the domain of this particular study. Instead, what this research can certainly affirm is a reasonably direct relationship between body weight and blood flow in the brain.
George Perry, Editor-in-Chief of the Journal of Alzheimer’s Disease, suggests this new research offers strong evidence to show how the brain can be directly influenced by broader physiological changes. This affirms the potential for lifestyle interventions in middle-age to play a major role in reducing a person’s risk of cognitive decline in later years.
“Acceptance that Alzheimer’s disease is a lifestyle disease, little different from other age-related diseases, that is the sum of a lifetime is the most important breakthrough of the decade,” says Perry, who did not work on this new study. “Dr. Amen and collaborators provide compelling evidence that obesity alters blood supply to the brain to shrink the brain and promote Alzheimer’s disease. This is a major advance because it directly demonstrates how the brain responds to our body.”
The new study was published in the Journal of Alzheimer’s Disease.
Source: IOS Press
Source of Article