British engineers are developing a modern version of the Negative Pressure Ventilator (NPV), more popularly known as the “iron lung,” to provide COVID-19 patients under the care of the NHS with a simple, inexpensive alternative to ventilators.
One of the resources that is in critically short supply for treating COVID-19 patients in need of respiratory support is ventilators. They help to support breathing in people whose lungs have been heavily affected by the virus, but these machines face a number of problems.
The most obvious difficulty is that ventilators are in short supply across the world as health authorities scramble to secure enough to meet the current and estimated demand as the pandemic spreads. They are also complex, expensive, require monitoring by trained personnel, and are dangerous to use on even healthy people because they require the patient to be intubated and sedated, and sometimes even paralyzed.
Such Intermittent Positive Pressure Ventilators (IPPV), as they are formally known, work by means of positive pressure. That is, they pump air or oxygen directly into the lungs as a way to help a patient breathe. The iron lung is essentially the opposite.
First suggested in the 17th century, an iron lung, in its classic form, is a large, airtight cylindrical chamber big enough to hold a person, whose head sticks out at one end through a special collar. Inside the chamber is a diaphragm hooked to an electric motor. As the motor turns, it operates a crank that causes the diaphragm to expand and contract. As it does so, the volume inside the chamber becomes larger and smaller, causing the air pressure to rise and fall. This causes the patient’s chest to expand and contract, allowing them to breathe even if they are totally paralyzed.
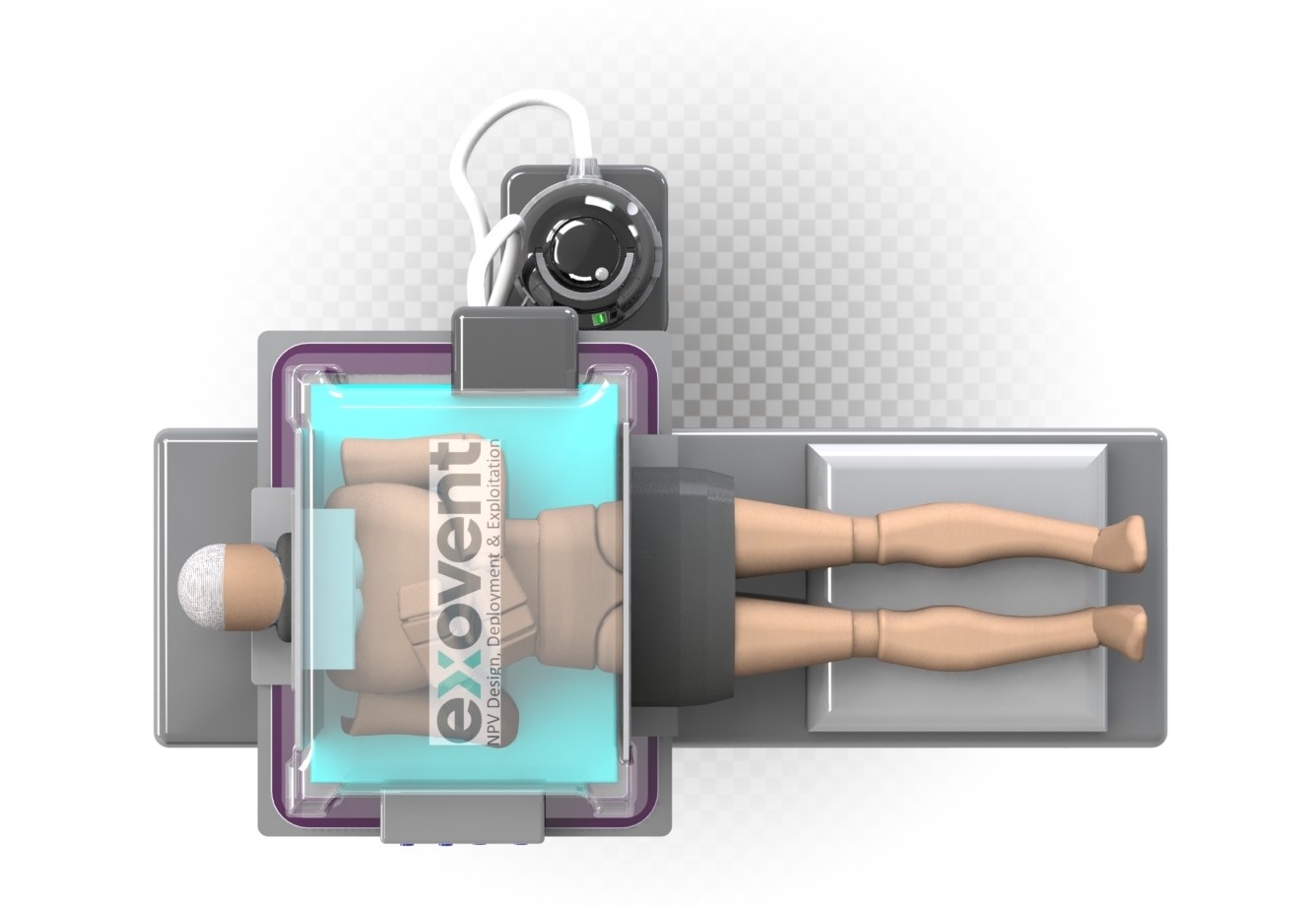
John Hunter/Steer Energy
Such iron lungs were a common sight in hospitals and even private homes during the height of the polio epidemics of the 20th century, though they have since been superseded by more sophisticated machines. But COVID-19 might give them a new lease on life.
The product of the University of Warwick, Marshall Aerospace & Defence Group, the Imperial NHS Trust, the Royal National Throat Nose and Ear hospital, and teams of citizen scientists, medical clinicians, academics, manufacturers, and engineers, the new NPV device, called the “exovent,” has already reached the prototype stage and will be tested at two intensive care clinics in the UK.
Unlike ventilators, the exovent doesn’t require intubation and is much simpler in design and operation. According to the consortium responsible for its design, patients can remain awake, take medications, eat and drink, and talk to their loved ones on the phone. In addition, the machine improves heart efficiency by 25 percent over conventional ventilators, which can adversely affect cardiac functions.
The developers also say that the exovent can be used in regular wards, which frees up ICU beds for more serious cases. Enclosing only the thorax, the machine does not use compressed air or oxygen, has only a few moving parts, and the components are readily available. The design is also adaptable for individual patients.
It’s estimated that, once approved, 5,000 exovents could be manufactured a week in the UK.
“We are delighted to be working with exovent to help scale up their non-invasive ventilator from prototype to volume manufacturing,” says Margot James, Executive Chair, Warwick Manufacturing Group (WMG), University of Warwick. “Our engineers and researchers are collaborating with the exovent team on the design, engineering, component sourcing and assembly of the ventilator. I am extremely proud of the unstinting and dedicated efforts of our research team, led by Archie MacPherson at WMG, and glad that we are able to apply our expertise to this important project.”
Sources: University of Warwick, Marshall Aerospace & Defence Group
Source of Article