More than 18 months ago a global COVID-19 vaccine roll-out commenced, beginning the biggest international immunization campaign seen in decades. Since then, the virus that causes COVID-19 has mutated significantly and health authorities have been discussing whether it is finally time to update our vaccines.
Over the last month advisory groups to the World Health Organization (WHO) and the US Food and Drug Administration (WHO) have delivered divergent recommendations for vaccine booster formulations. The differing advice is a potent reminder of how uncertain the road ahead is as the COVID-19 pandemic moves through its third year.
Following the emergence of the Omicron SARS-CoV-2 variant at the end of 2021, the dominance of this new viral variant quickly became clear. However, the spread of Omicron over the past six months has not been a straightforward process.
When it was first characterized in November 2021 the WHO actually rolled three separate viral subtypes under the one Omicron umbrella: BA.1, BA.2 and BA.3. These three sub variants were all relatively distinct, but BA.1 was the first iteration to really take hold around the world.
Since last year, Omicron has undergone a plethora of changes and mutations. Scores of distinct subtypes have been characterized, and waves of infections have ebbed and flowed as newer versions of the virus took hold – from initial BA.2 spread to BA.2.12.1 and then BA.4 and BA.5.
The sheer pace of new sub variants emerging and becoming dominant mean global health authorities are faced with an impossible decision. How do we target new vaccine formulations when it is likely entirely novel SARS-CoV-2 iterations will be spreading by the time the doses are made and administered?
In mid-June the WHO’s Technical Advisory Group on COVID-19 Vaccine Composition (TAG-CO-VAC) met to discuss this very issue. An interim statement from the advisory group indicated the current formulation of the vaccine was still incredibly effective at reducing severe disease outcomes from COVID-19, so that should still be used as a primary protocol for those yet to be vaccinated.
But, the group did recognize SARS-CoV-2 is incrementally changing its form, and there is value in a booster that can broaden one’s immune response to emerging variants. Omicron, of course, was found to be the variant that a prospective booster should target, and two questions arose: What specific Omicron subtype should a booster aim for, and should the booster be monovalent (containing antigens solely for the targeted Omicron subtype) or bivalent (containing antigens for both the newer Omicron target and the original strain)?
On the latter question the WHO group indicated a monovalent booster would be the best course of action. The Omicron subtype decided upon as the target was BA.1, despite the fact that in most parts of the world it had already been supplanted by other Omicron iterations.
The advisory group’s thinking behind targeting BA.1 was that instead of trying to guess what specific kind of Omicron subtype will be dominant months into the future, it would be better to use the booster to give our immune systems a look at the most distinct form of the virus currently circulating. This would, hypothetically, broaden immunity against variants yet to emerge.
WHO
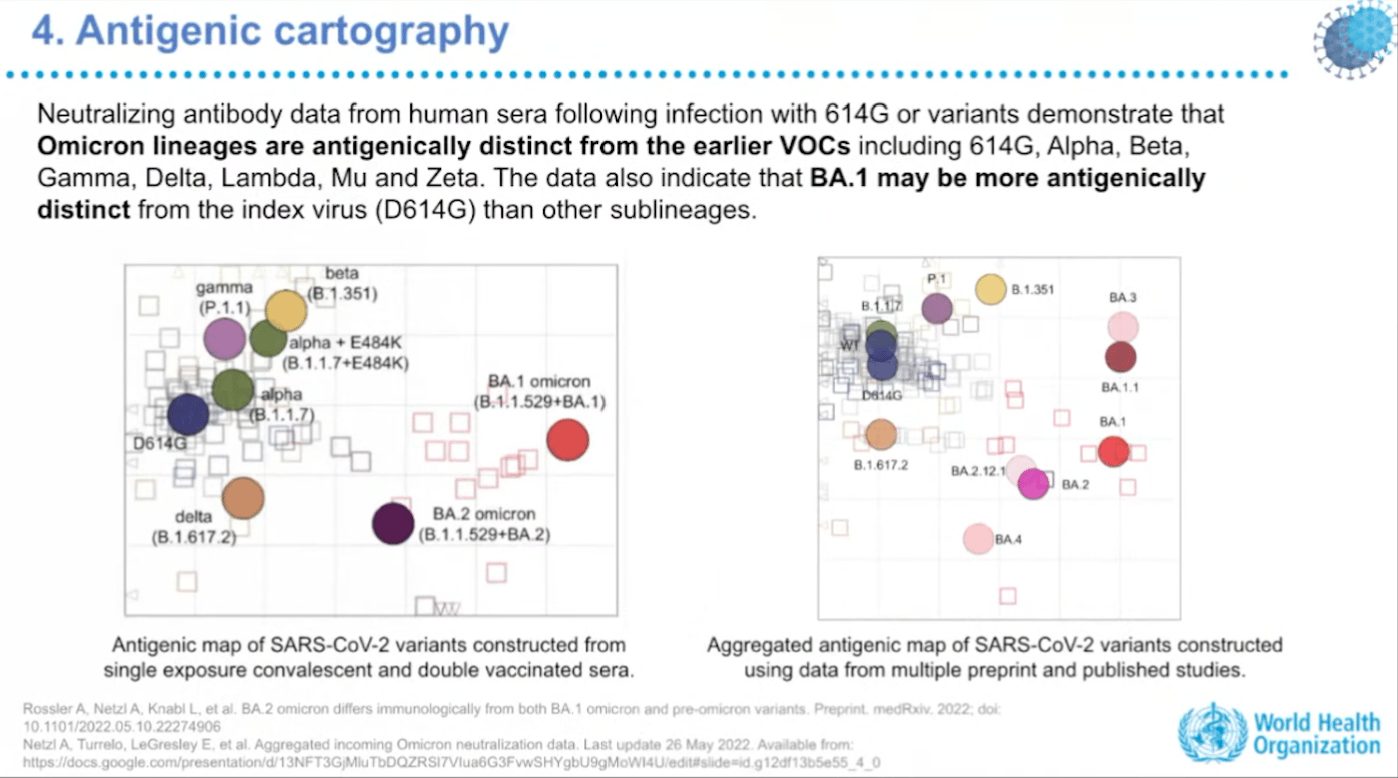
Data from the WHO showed the most antigenically distinct SARS-CoV-2 variant currently circulating is BA.1. Antigenic cartography, which maps SARS-CoV-2 variants in terms of how antigenically different they are from one another, suggested BA.1 is more distinct than other forms of Omicron, so it could be the best target for broadening immunity.
Speaking to CNN, Kanta Subbarao a virologist who chaired the June TAG-CO-VAC meeting, said the goal of booster strategies should not be to try and guess the leading future variant but to broaden immunity in the hopes of protecting people from what may arise.
“I still think there’s value in increasing the breadth of immunity and I will reiterate that we’re not trying to match what may circulate,” said Subbarao. “It is not so much to match what is likely to circulate because there’s so much uncertainty about the trajectory of this evolution. We’re trying to increase the breadth of the immune response without losing the benefit from the index vaccine that’s performed so well.”
At the end of June the FDA’s Vaccines and Related Biological Products Advisory Committee met to offer its recommendations for fall/winter COVID-19 vaccine formulations. The long meeting included presentations from both Pfizer and Moderna, who offered new data on BA.1 boosters that have been in development since the beginning of the year.
This new data from Pfizer and Moderna showed the BA.1 boosters in development produced strong immune responses to Omicron compared with the original vaccine formulation. However, immune responses generated by BA.1 boosters against BA.4 and BA.5 was not as strong.
The committee ultimately only voted on a general question asking whether “an Omicron component” be added to COVID-19 booster vaccines. The recommendation was nearly unanimous (19 to 2), while the discussions seemed to focus on the BA.4 and BA.5 variants that are rapidly becoming dominant in the United States.
A formal announcement from the FDA the following day revealed the final decision, and it directly contrasted with the WHO recommendation. The FDA will require COVID-19 boosters to be bivalent, and contain antigens targeting the BA.4/5 subtype of Omicron.
“Following the vote, and striving to use the best available scientific evidence, we have advised manufacturers seeking to update their COVID-19 vaccines that they should develop modified vaccines that add an Omicron BA.4/5 spike protein component to the current vaccine composition to create a two-component (bivalent) booster vaccine, so that the modified vaccines can potentially be used starting in early to mid-fall 2022,” said Peter Marks, director of the FDA’s center for biologics evaluation and research.
The divergent decisions leave vaccine makers in a tough position. Both Pfizer and Moderna have already begun manufacturing BA.1 booster doses. Pfizer in particular has indicated it was ready to begin distributing BA.1 boosters immediately, while Moderna claimed to have 200 million doses in the pipeline for early September. The FDA decision to target BA.4/5 means there will be a delay, pushing any US booster program back to October or even November.
It’s also unclear what will happen to any pre-existing supply of BA.1 boosters. Will they be distributed anywhere? And if so, what kind of confusion could ultimately result if multiple different COVID-19 vaccine formulations started to roll out around the globe. No announcement has come from Pfizer or Moderna as to whether they will continue manufacturing of BA.1 boosters for other regions in the world.
Moving forward it is obviously necessary for some kind of central global authority be formed to track and recommend COVID-19 vaccine variant targets in much the same way influenza vaccines are annually reformulated. Twice a year the WHO convenes a meeting with seven different influenza surveillance organizations around the globe. It is here that recommendations are made for influenza vaccine composition for the Northern and Southern Hemisphere winters.
Jerry Weir, director of viral products at the FDA, has called for improved global co-ordination and consensus on COVID-19 vaccine reformulations in the future. He does note that the current process for influenza vaccines evolved over decades so it is unsurprising there is such a discordancy right now with SARS-CoV-2 discussions.
“I will remind you that the parallel track of influenza strain selection, which works very well, was a process that was honed over many, many years,” added Weir. “This is a very different virus, so we probably have a lot of work to do on this strain selection process for COVID vaccines.”
Source of Article